GLUT-5 and co: what happens in the body
Letzte Aktualisierung am 9. September 2024 von Dr. Michael Zechmann-Khreis
This article is somewhat more complex and requires some prior knowledge of biological processes and terms. It deals with transport proteins such as GLUT-5 and SGLT, cell membranes and the absorption of substances in cells. But don’t worry: you don’t need to understand all of this if you want to get your fructose malabsorption and its symptoms under control.
GLUT and SGLT: transport proteins at a glance
Transport proteins (carrier proteins) are proteins that transport specific substances through cell membranes. GLUT stands for “glucose transporter”, while SGLT is the abbreviation for “sodium-glucose linked transporter“, i.e. “sodium-dependent glucose transporter”. The exact physiology and function of these transport proteins are not yet fully understood, particularly the mechanisms by which different types of sugar are absorbed into the body. This is a hotly debated topic among experts. The current state of research is summarized below, particularly with regard to intestinal fructose intolerance.
Absorption of sugars from the chyme
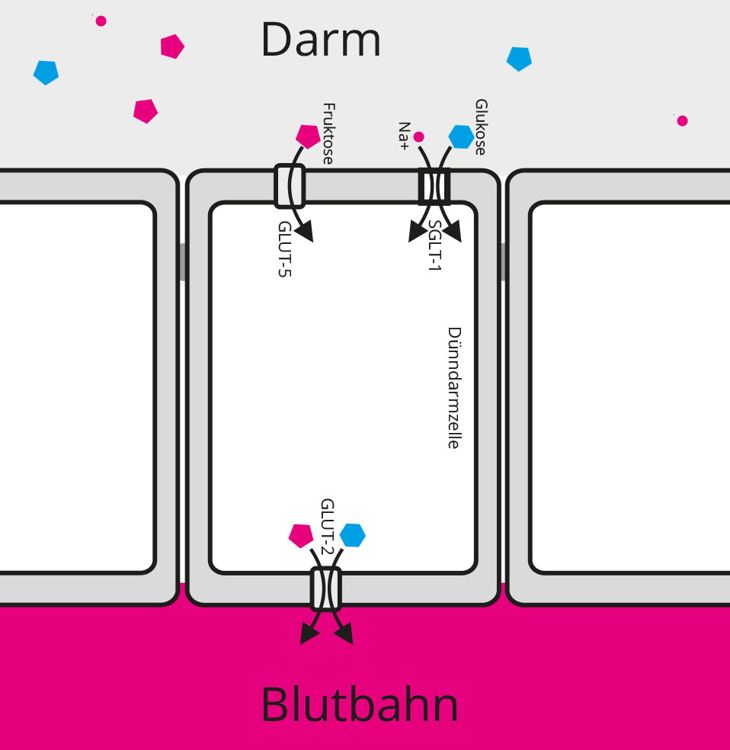
The cell membrane serves as a barrier that prevents foreign substances from entering the cell. However, as the body needs to absorb and release nutrients, there are various mechanisms for transporting these substances through the cell membrane. Transport proteins can actively or passively channel substances through the cell membrane of the brush border cells (enterocytes). Additional factors are often necessary for this. The SGLT-1 transporter, for example, requires the sodium ion (Na+). This ion binds to the transporter, causing it to change its shape and the glucose is transported through the cell membrane together with the sodium. The sodium acts like a key that opens the door for the glucose.
Transport proteins are dynamic
Transport proteins are not fixed constants. There is no fixed number of precisely defined locations in the small intestinal mucosa. They are produced according to demand, time of day and age. At high fructose concentrations in the chyme, for example, the SLC2A5 gene is activated to form mRNA*, which is then translated into GLUT-5. This allows fructose to be absorbed. The body reacts to the food supplied by starting the corresponding absorption mechanisms. GLUT proteins are therefore formed depending on the sugar concentration in the chyme and transport the sugars into the small intestine cells and finally into the blood. They are not firmly anchored in the cell membrane, but can change their position (translocate).

As described above, the number of GLUT-5 transporters also depends on the fructose concentration in the food3). GLUT-5 absorbs the fructose from the food pulp and brings it into the small intestine. From here, the fructose enters the bloodstream via GLUT-2 transporters. However, GLUT-5 is not only produced in response to fructose in the diet, but is also subject to a circadian rhythm2). In rats, for example, GLUT-5 is produced significantly more at the end of the day than at the beginning of the day1) and so it is possible that the time of day also plays a role in humans. GLUT-7 can also absorb fructose from food5), but appears to play a subordinate role in the absorption of fructose. GLUT-2 transports glucose very effectively, but also fructose, mannose or galactose. This transporter is mainly found in liver cells, but also in many other organs, such as the small intestine. Here it is primarily responsible for transporting glucose and fructose out of the small intestine and into the bloodstream. SGLT-1 transports glucose, but not fructose.
Why does glucose help with fructose absorption?
If a lot of glucose is ingested with food, GLUT-2 transporters can migrate (translocate) to the cell wall on the small intestine side or be formed directly on this side of the cell. As these GLUT-2 transporters can also absorb fructose, they relieve the GLUT-5 transporters and help to absorb fructose from the intestine.
How does fructose intolerance develop?
Now the important question arises as to which mechanism is disturbed in fructose intolerance. What is the reason for intestinal fructose intolerance? Are the GLUT-5 transporters not working properly? Are there too few of these vans? Is the signal transmission not working and is therefore too little mRNA and consequently too few transporters being produced? Or is fructose absorption disturbed in another way?
We don’t know the answer (yet)! Anything is possible. It is also possible that there are different problems that together cause the clinical picture of intestinal fructose intolerance. So perhaps there are two or three reasons, or perhaps a previously unknown mechanism is to blame for the malabsorption of fructose. A great deal of research work is still required here in the coming years.
Sorbitol (E420) blocks GLUT-5?
It is often stated that sorbitol blocks GLUT-5 and should therefore be avoided in cases of intestinal fructose intolerance. Experience shows that sorbitol (and other sugar alcohols) actually has a negative effect on fructose intolerance and fructose absorption. However, scientific evidence, especially for the underlying mechanism, is still lacking. Nevertheless, these sugar alcohols should be avoided.
What we know today
Basics of the “glucose trick”
We know from the processes described above that dextrose (glucose) helps to absorb fructose:
- On the one hand, high glucose concentrations in the intestine cause GLUT-2 transporters to migrate to the luminal (apical) wall and, since they also transport fructose, they increase fructose absorption from the intestine.
- On the other hand, glucose may have a positive effect on the formation of GLUT-5
- Fructose intake stimulates the formation of GLUT-5, which means that completely abstaining from fructose would worsen fructose intolerance, as the body lacks the reason to form GLUT-5.
- Sorbitol should be avoided as it is suspected of inhibiting fructose absorption by inhibiting the GLUT-5 transporter. Exactly how this mechanism works has not been clarified, but experience shows that there are correlations.
- Fructose is better tolerated by many patients in the afternoon, which could be related to the circadian rhythm of GLUT-5 expression.
- High-fat food improves fructose absorption because it slows down the intestines. This means that the chyme has a longer residence time in the intestine. The few transporters can thus work longer and absorb more fructose.
Text explanations: mRNA is the abbreviation for messenger RNA. This is the copy of a specific gene segment that is created in the cell nucleus and from which a protein can then be produced via various processes.
Sources
(1) Castello A, Guma A, Sevilla L, Furriols M, Testar X, Palacin M, Zorzano A. Regulation of GLUT5 gene expression in rat intestinal mucosa: regional distribution, circadian rhythm, perinatal development and effect of diabetes. Biochem J 1995; 309 (Pt 1): 271-277 63
(2) Corpe, C.P., Burant, C.F., 1996. Hexose transporter expression in rat small intestine: effect of diet on diurnal variations. Am. J. Physiol. 271, G211-G216.
(3) Jiang, L., David, E.S., Espina, N., Ferraris, R.P., 2001. GLUT-5 expression in neonatal rats: crypt-villus location and age-dependent regulation. Am. J. Physiol. Gastrointest. Liver Physiol. 281 (3), G666-G674.
(4) Wright EM, Martin MG, Turk E. Intestinal absorption in health and disease–sugars.
Best Pract Res Clin Gastroenterol 2003; 17: 943-956
(5) Li Q, Manolescu A, Ritzel M, Yao S, Slugoski M, Young JD, Chen XZ, Cheeseman CI. Cloning and functional characterization of the human GLUT7 isoform SLC2A7 from the small intestine. Am J Physiol Gastrointest Liver Physiol 2004; 287: G236-G242
(6) Drozdowski Laurie, Thomson Alan. Intestinal sugar transport. World J Gastroenterol 2006 March 21; 12(11):1657-1670
(7) Mueckler Mike, Thorens Bernard. The SLC2 (GLUT) family of membrane transporters. Molecular Aspects of Medicine 34 (2013) 121-138
